Definition and Causes:
A clinical state defined as decreased production of thyroid hormone, by the thyroid gland resulting in the deficiency of circulating hormone which regulates essential functions such as heart rate, digestion, physical growth, and if left untreated, leads to multiple organs and tissues damage.
The hormone is a chemical released by the cells and functions as a messenger that transport signals to other cells. The thyroid gland is situated in the lower part of the neck. It lies in front of the windpipe (or trachea; tra-key-ah) below Adam’s apple.
The gland produces 2 thyroid hormones called thyroxine (abbreviated T4) and triiodothyronine (abbreviated T3). The release of these hormones is partly regulated by
- Other glands such as the pituitary and hypothalamus, situated within the brain, and
- By the circulating thyroid hormones itself via negative feedback (the latter refers to the ability of a circulating hormone to switch off its own production to avoid excessive levels or increase production in case of deficiency)

Hypothalamus (an area at the base of the skull within the brain) releases a hormone known as thyrotropin-releasing hormone (TRH).

The rate of production is controlled by the amount of hormone circulating within the body, and in turn by the pituitary glands.
An insufficient amount of hormone triggers increase the release of TSH.
The excess amount of hormone triggers decrease the release of TSH.

Causes:
1) Hashimoto’s thyroiditis:
Most common cause of hypothyroidism is an autoimmune disease in which the body’s immune system attacks the thyroid tissue and develops antibodies to an enzyme called thyroid peroxidase (anti- TPO antibodies). It usually runs in families and is 5-10 times more common in females.
It is identified by detecting anti-TPO antibodies in the blood or by performing a thyroid scan.
2) Treatment of hyperthyroidism:
Individuals producing thyroid hormone in excess (hyperthyroidism); when treated with anti-thyroid drugs to normalize the thyroid levels, may result in permanent hypothyroidism.
3) Radiation therapy:
Used to treat head and neck cancers may have an effect on the thyroid gland and may cause hypothyroidism.
4) Thyroid surgery:
If the gland is removed totally or partially; it may result in decreased or no production of thyroid hormone resulting in hypothyroidism.
5) Pituitary or hypothalamic disease:
Any defect in signaling the thyroid gland; to produce thyroid hormone by the pituitary or hypothalamus may result in deficient levels.
6) Severe iodine deficiency: cause hypothyroidism
7) Medications:
To treat a psychiatric disorder such as lithium may cause hypothyroidism.
Symptoms:
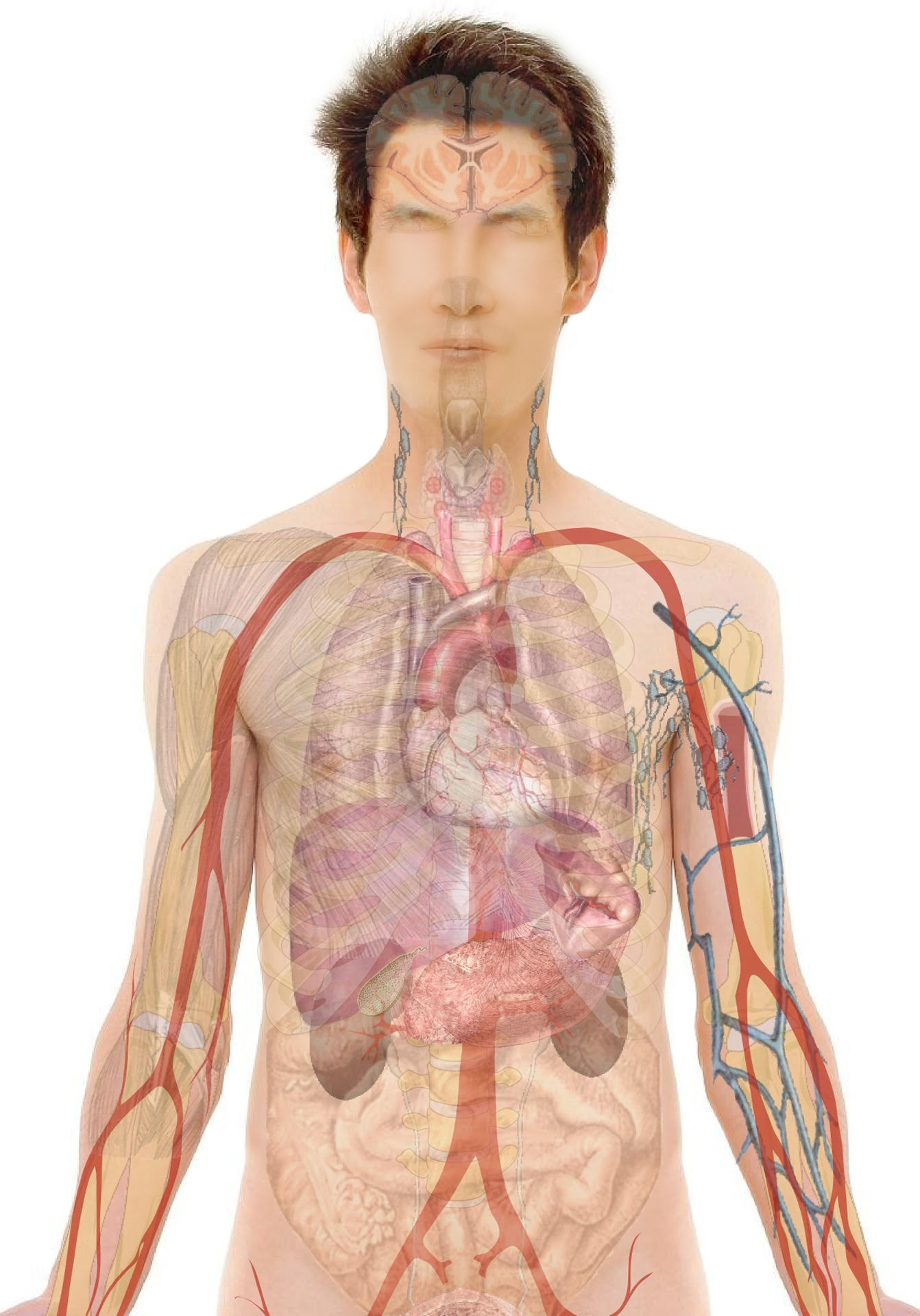
Clinically the disease varies from one patient to the other depending upon cause, duration, and severity of the hypothyroid state. Since thyroid hormones influence most organs, tissues, and cells of the body, there can be a wide spectrum of signs and symptoms in this disorder (see figure).

Note: An endocrinologist (doctor specializing in hormonal diseases) would most likely recognize the subtle manifestations and would be more skilled to do physical thyroid gland examination. Consultation is recommended for:
- Patients of age ≤18 years
- Patients who do not respond to treatment
- Pregnant patients
- Cardiac patients
- Structural changes in the thyroid gland
- Presence of other endocrine diseases
Investigations and Treatment:
History and Physical:
Although history and physical examination will provide definitive information in severe cases, asymptomatic individuals with non-specific signs and symptoms may present.
The disease should be considered in older females and in pregnancy.
Common symptoms may include the following:
- Fatigue
- Dryness of skin
- Constipation
- Hoarseness of voice
- Cold intolerance
- Weight gain
Labs:
- A blood test is always needed to confirm the diagnosis
- The measurement of thyroid hormone is usually decreased unless it is early in the disease course
- Thyroid-stimulating hormone (TSH) is measured in the early phase which should be elevated
Once the hypothyroidism is confirmed the underlying cause of the disease is determined by:
- Patient’s symptoms
- Local thyroid gland examination
- Presence/ absence of antibodies
MRI of the brain:
This does not use x-rays. Instead, MRI uses magnetic fields over the body. The device looks like a long cylindrical tube. Patients will lie on a table that slides into the hollow tube. Computer analysis of magnetic fields within the machine can generate images of the internal structures of the body’s organs, including the brain. MRI of the brain will show the normal structures, plus any area(s) of brain injury caused by the inflammation, tumors, etc. Patients must lie still inside an MRI machine for about 30-45 min. In some circumstances, a dye might be injected into the veins (enhanced MRI) just before the scan to help improve the detection of abnormalities. Patients who complain of claustrophobia or discomfort may be given a mild sedative to help relax prior to MRI scanning. The test may be advised by the doctor to exclude other causes if necessary.
TREATMENT:
Goal: Restore normal thyroid state.
Treatment: Is individualized, considering age, weight cardiac status
Monitoring: Every 6 to 8 weeks until TSH is normalized, then at 6 months, then annually
Agent of choice:
- Levothyroxine once daily, on an empty stomach
Medical conditions that may interfere with thyroid hormone absorption:
- GI malabsorptive disorders
- Previous small-bowel bypass surgery

Risk Factors and Prevention:
Risk factors
- Females ≥50 years of age
- Stress
- Family history of autoimmune disease
- Previously treated with anti-thyroid medication or had radioactive iodine
- Received radiation therapy to the head or neck region for cancer
- If thyroid has been removed surgically
- Have an autoimmune disease such as diabetes
Outcome:
- Thyroid hormone replacement therapy continues for life
- Usually, thyroid levels return to normal with proper treatment
Complication:
The most severe form of hypothyroidism “myxedema coma” is a rare complication, caused by an infection, illness, exposure to cold, or certain medications in people with untreated hypothyroidism. Myxedema coma can result in death.
Alert: Seek medical help immediately in case of:
- Chest pain
- Infections
- Symptoms which are getting worse
- Newly developed symptoms